Patient Information
Aspiration
An aspiration is a procedure where we remove a small amount of fluid from an area like a joint using a needle under ultrasound guidance. This is a common procedure often performed on a “Baker’s cyst” of the knee.
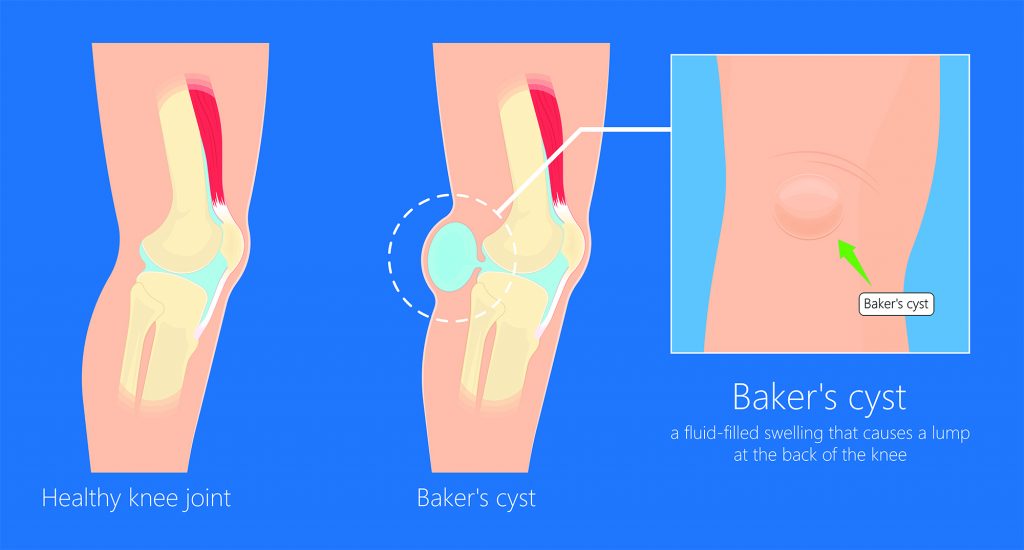
By removing swelling from a structure like the knee, it allows us to reduce the pressure in the joint which can give you symptomatic relief. It also allows us to inject other constituents in the space afterwards like steroids, PRP or Hyaluronic acid without increasing the total volume of fluid in the joint.
The information below tells you what is involved and what the possible risks are of having an aspiration. It may not answer all your questions, so if you have any queries or concerns, please do not hesitate to contact us.
Why should I consider this procedure? If you have a swelling in or around a joint, it may be very painful and limit your mobility. Removing this fluid will result in less pain and increased mobility. If the fluid accumulation is in a muscle eg from a large tear, then removing the fluid will allow the muscle fibres to come back together to heal faster. Occasionally fluid taken out of a joint may need to be be sent for further testing. We will discuss this further should it be required at the time of the procedure.
At the appointment:
The clinician will first perform an ultrasound scan to assess the condition again and to ensure this procedure is still indicated. They will use ultrasound to locate the precise part of the joint or muscle to be aspirated.
We use an aseptic ‘no touch” technique to insert a fine needle into the joint or muscle and remove a small amount of fluid from the area in a syringe. This will usually give you immediate relief of the symptoms you are experiencing.
It’s best to take it easy on the area for the next few hours after the procedure. If the area feels uncomfortable, using ice or over the counter anti-inflammatory medications will help settle it down.
Risks of the Procedure:
An aspiration is a common procedure that has little risk.
As with any injection into the body, there is always a risk of infection. This is extremely rare across all injections administered in all healthcare settings. Around 1:50,000 patients may get an infection according to the literature following an injection procedure. The risk is similar to having a standard blood test.
Every precaution is taken to avoid infection including a “no touch” aseptic technique to ensure your safety during the procedure. However if the joint becomes red, warm or tender, or if you develop a fever in the 5-7 days post procedure please go to your local Accident & Emergency Department and inform them of the procedure you have had done.
When you have an injection there is a potential for injury or trauma to nerves, blood vessels or soft tissue structures. The clinician uses ultrasound guidance and is trained to take all appropriate steps to minimise risks and avoid injecting or traumatising any soft tissue structures when performing the injection. However with particular injections at certain locations there will always remain a very small risk that this could occur. This will be discussed further at your appointment.
If you are taking Warfarin or other blood thinning drugs we may need to discuss the procedure with your GP.
Does it hurt?
Not really! There may be a bit of discomfort at the time of the injection procedure, but Ultrasound guidance means that injections can be delivered much more accurately and comfortably.
